When we talk about menopause, gut health probably isn’t the first thing that springs to mind. But it absolutely should be. Why? Because your gut and your emotions are closely connected – and if your gut is struggling, your mood often is too.
Surprised? You’re not alone. But here’s the scoop: around 90% of serotonin, your body’s feel-good chemical, is produced in the gut. Yep – your happy hormone is hanging out in your belly.
And yet, gut health is often overlooked when it comes to menopause symptoms. So let’s change that.
Following are 12 signs your gut could be asking for a little more love, especially during perimenopause or post-menopause.

12 signs your gut might need some TLC
- Anxiety
- Bloating
- Brain fog
- Constipation/diarrhoea (or both)
- Depression
- Digestive issues (obviously!)
- Feeling unwell often
- Food sensitivities (especially to gluten or dairy)
- Forgetfulness
- IBS
- Mood swings
- Skin issues like eczema and acne
How many of these sound familiar?
While this list can’t definitively diagnose gut problems, it’s a strong indicator that your digestive health could use some attention. Let’s dig into why this matters – especially during menopause.
Your gut: more than just your stomach
When we say “gut”, we’re talking about your entire digestive system. That includes your mouth, oesophagus, stomach, small and large intestines, pancreas, liver and gallbladder. It’s a beautifully complex system that does more than just digest your food.
In fact, your gut lining is part of your immune system, helping defend against invaders. It’s no wonder researchers refer to it as the “second brain.” Ever heard phrases like “trust your gut” or “gut instinct”? Turns out they’re based in science!
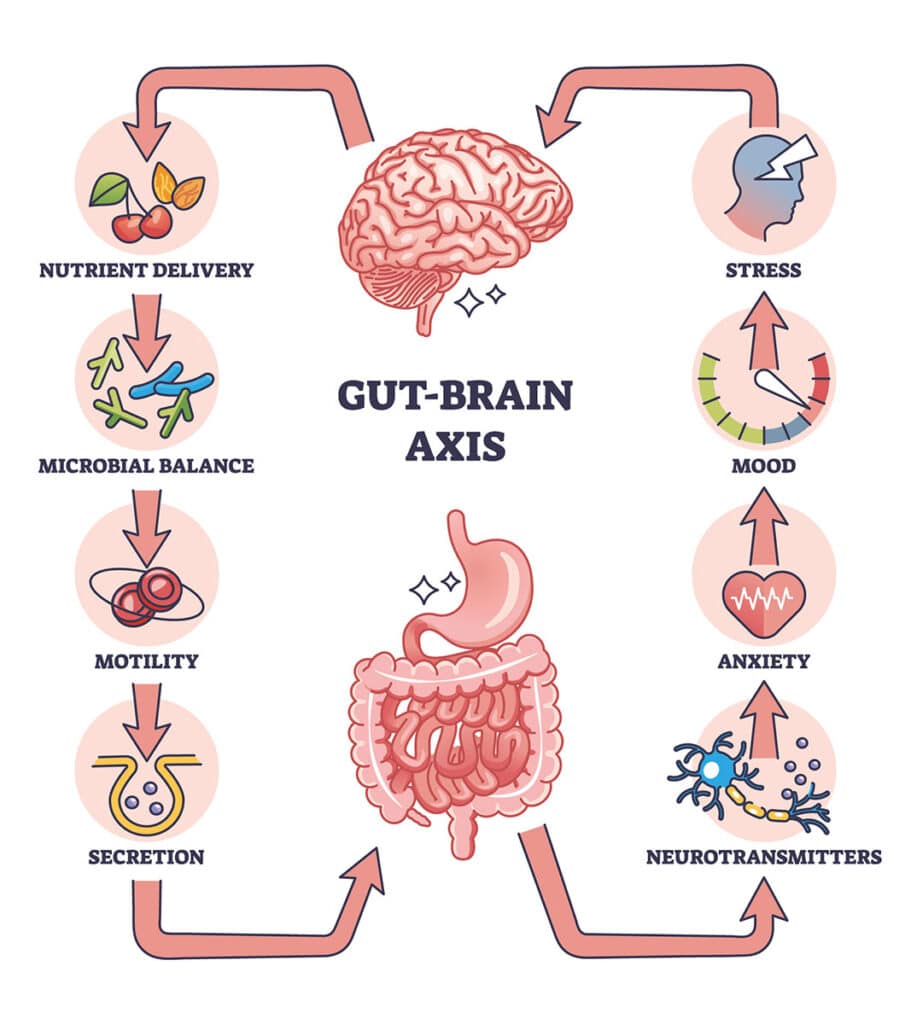
The gut-brain axis: a two-way conversation
One of the most fascinating discoveries in recent years is the gut-brain axis – the ongoing communication between your digestive system and your nervous system.
Your gut has its own mini nervous system called the enteric nervous system, and it talks to your brain all day long. So when stress hormones like cortisol increase, your digestion can slow right down. Cue: constipation or other digestive upsets.
That’s why stress, low mood, or anxiety during menopause can show up as bloating, IBS or even food sensitivities. Isn’t that amazing?!
Gut health and menopause: what’s the link?
Your gut is home to trillions of microbes – aka the microbiome. These friendly bugs help digest food, produce vitamins, balance hormones, and keep inflammation in check.
A balanced microbiome also supports:
- Estrogen metabolism
- Mood regulation
- Immune function
- Clear skin
- And more!
But if your gut health is out of balance – what’s known as dysbiosis – your body may struggle to absorb the nutrients it needs. And that can trigger a domino effect.
One of the first signs? Changes in how often (and how easily) you go to the loo. Yep, your elimination habits – we’re talking poop – are a big deal. Ideally, you want to be regular and consistent. Why? Because pooping is one of yur body’s key ways of clearing out excess hormones, toxins and waste.
In fact, recent research published in the Menopause Journal found that constipation and elimination issues are linked to more severe menopause symptoms2. That’s a big clue that your gut is playing a major role in how you feel.
What’s more, if dysbiosis sticks around, it can lead to increased gut permeability, often called leaky gut. This means that tiny particles like toxins, bacteria, and even proteins (such as gluten) can pass through the gut lining into your bloodstream – potentially leading to inflammation and worsened menopause symptoms.
Whether you’re riding the rollercoaster of mood swings, battling fatigue, headaches, anxiety, depression, or facing stubborn weight gain, it’snot just your hormojnes that could be at play – your gut health could be a hidden culprit.
And that’s a lot of reasons behind why we created Happy Go Tummy® – your daily ally for digestive harmony and a smoother menopause journey. 💙
9 daily habits to support your gut during menopause

Ready to give your gut some love? These daily habits can restore balance and improve how you feel. 💙
- Stay hydrated – water helps digestion flow smoothly.
- Eat more high-fibre foods – think fresh fruit and veggies, legumes and whole grains like quinoa, and brown rice. (Chia seeds are amazing.)
- Cut back on sugar and processed foods – the bad bugs love these.
- Add fermented foods – like kefir, sauerkraut, miso, kimchi, plain yoghurt.
- Chew slowly and often – good digestion begins in your mouth so make good use of the enzymes in your saliva to help with the food breakdown process.
- Rest and digest: the tummy loves a good break, especially at night so try to close the kitchen three to four hours before bed.
- Try a good quality probiotic – the good bugs your gut wants more of
- Embrace prebiotic – prebiotics are the indigestible fibre probiotics need to thrive and survive.
- Run, don’t walk to get your hands on Happy Go Tummy® – it’s a synbiotic. This means it’s prebiotic/probiotic combination supplement so you’re ticking off points 7. and 8. right there.
Happy Go Tummy® contains award-winning Livaux® which is a prebiotic from Kiwifruit pectin. This four-minute video will tell you more about Livaux®’s incredible benefits.
Jane’s story: a gut feeling that changed everything
Meet Jane, a successful career woman.
She’s always been a go-getter, but as menopause crept in, she felt like her body and mind were in turmoil. Her energy levels plummeted, mood swings became the norm, and her sleep patterns became erratic. Jane knew she needed a solution, and that’s when she began her quest to balance her menopausal symptoms by optimising both her hormones and her gut health.

Jane had read about the scientific studies that show a strong connection between gut health and mental wellbeing as well as the influence of the microbiome on mood and emotions.
And she understood the importance of nurturing her gut microbiome as well as her hormones to alleviate her menopausal discomfort.

Her first step was to consult with a holistic menopause and gut health specialist. She developed a holistic plan with their guidance that included dietary changes and lifestyle modifications to support her gut health. She also began taking MenoMe®’s Perky Post® for hormonal support and Happy Go Tummy®, a high-quality synbiotic prebiotic/probiotic combination.
As a result of her dietary changes, Jane’s diet was enriched with fibre as well as probiotics and prebiotics, which together with Happy Go Tummy® helped her nurture a balanced gut microbiome.
She also incorporated stress-reduction techniques like yoga and meditation to foster a healthier mental state for that all-important gut-brain axis.
As the weeks passed, Jane experienced remarkable improvements. Her mood swings became less frequent, her anxiety levels decreased, she experienced far less bloating and the clogged feeling of constipation disappeared.
And by taking care of her gut, Jane discovered first-hand that she was more equipped to deal with the emotional rollercoaster of menopause.

The bottom line 💙
Your gut isn’t just where your food goes – it’s a powerful part of your overall health, especially during menopause. If you’re ticking off several symptoms from the list above, it could be time to show your gut some love.
Because when your gut is happy, your hormones, mood and whole body are happier too.
Disclaimer: Our articles are guidelines only and should never be taken as medical advice. Any signs and symptoms you’re experiencing could be due to a number of reasons. If you’re experiencing ongoing signs, please see your health professional.
And just so you know: this blog is written by a real person who has studied the physiology of menopause and women’s healthy ageing. While we may use AI as an assistant, the research, insights and heart behind every piece comes from us.
Share with a friend
Sign up to our mailing list for the latest news and stories and receive a $5 discount code to redeem on your first purchase, plus receive a 3-step eBook on ways to support your body through menopause.
This site is protected by reCAPTCHA and the Google Privacy Policy and Terms of Service apply.
Related Articles
Resources
- Appleton J. The Gut-Brain Axis: Influence of Microbiota on Mood and Mental Health. Integr Med (Encinitas). 2018 Aug;17(4):28-32. PMID: 31043907; PMCID: PMC6469458
- Exploration of the association between menopausal symptoms, gastrointestinal symptoms, and perceived stress. https://www.menopause.org/docs/default-source/press-release/menopause-symptoms-associated-with-gastrointestinal-symptoms.pdf
Disclaimer
Our articles are a guideline only and should not take the place of medical advice. Any signs and symptoms you are experiencing could be due to a number of reasons. If you’re experiencing ongoing signs please see your health professional.