Post-menopause is often framed as an ending. The finish line after a long and frequently exhausting race. But ask women who are living it well, and a different picture emerges — one of clarity, focus, and a genuine shift in what matters.
That doesn’t mean post-menopause is without challenges. Lower estrogen affects more body systems than most women are told, and some symptoms that started in perimenopause don’t simply switch off. But post-menopause is also a stage where the right knowledge and the right support make a real, measurable difference. This is where thriving becomes less about luck and more about intention. Hallelujah!
What is post-menopause?
Post-menopause begins after 12 consecutive months without a period, as long as there’s no other medical cause. From that point, estrogen and progesterone stabilise at lower levels – the intense hormonal fluctuations of perimenopause settle, and the body finds a new baseline. How good is that?
Most women reach this stage between 45 and 55, though surgery, medical treatment, or genetics can bring it earlier. The average in the Western world is 51. Once there, a woman remains in post-menopause for the rest of her life. That sounds significant because it is, but it’s also simply a new hormonal rhythm, not a decline or deficiency.
 What’s happening in the body?
What’s happening in the body?
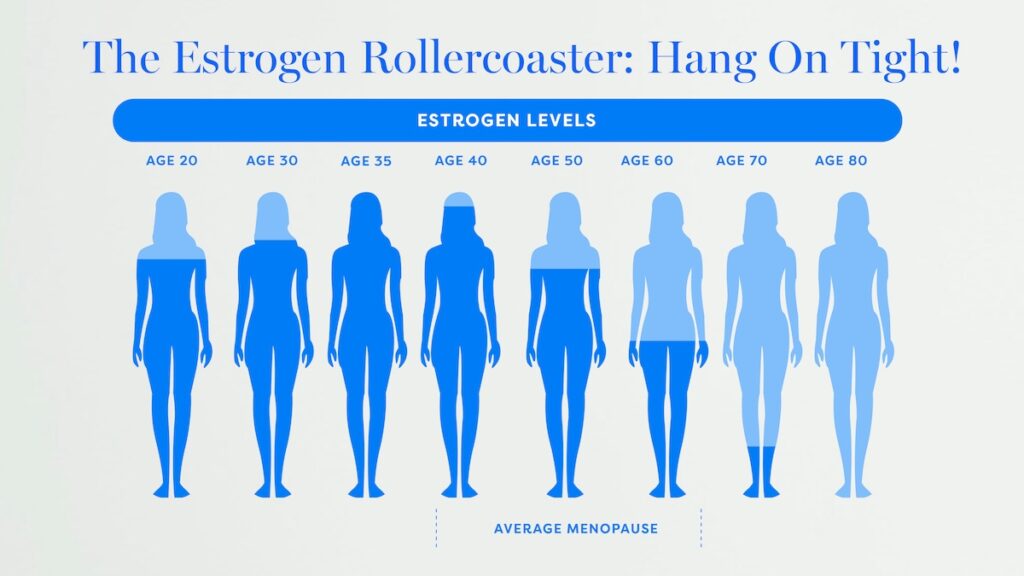
Estrogen does a lot more than just regulate periods. It influences bone density, heart health, metabolism, brain function, skin, connective tissue, vaginal and urinary tissues. In fact, I call it our juice. And when levels drop and stabilise at a lower point, all of these systems are affected to some extent.
That’s not intended to scaremonger, but it is a reason to understand what the body needs now, rather than applying the same habits that worked in your thirties and wondering why they feel less effective.
Signs and symptoms that can continue
Some women feel great once perimenopause is behind them. Others find that certain symptoms continue, evolve, or arrive for the first time in post-menopause.
Hot flushes and night sweats are often assumed to be over by this stage. Sometimes they are. The SWAN study, published in JAMA Internal Medicine, found that vasomotor (that’s hot flushes and night sweats) symptoms lasted more than seven years for over half the women studied, and persisted for a median of 4.5 years after the final period.
The Australasian Menopause Society estimates up to 80% of women experience them during the transition – and for some, they continue well beyond it. It should be noted that for women over the age of 60, this could be linked with hypertension.
Vaginal dryness and bladder changes – collectively known as genitourinary syndrome of menopause, or GSM – affect more than half of post-menopausal women according to studies, and unlike hot flushes, tend to worsen rather than improve. If intimacy is uncomfortable or bladder urgency is affecting daily life, that’s worth raising with your medical professional. The supplement D-Mannose is reputed to be helpful for recurrent UTIs (urinary tract infections), which can also arise.
Sleep disruption remains common, too. A 2024 meta-analysis covering nearly 30,000 menopausal women found poor sleep quality in 50.8% of participants. Jean Hailes for Women’s Health identifies it as one of the most commonly reported and most underaddressed symptoms of this stage.
Joint stiffness, hair thinning, changes in skin, shifts in body composition, and mood or concentration changes can all feature in post-menopause as well. The good news? Emotional symptoms – anxiety, low mood, mild memory fog often improve compared to perimenopause, but they don’t always disappear entirely. And good sleep, regular movement, and social connection all help with how good you feel.

Long-term health: what to know
Two areas deserve particular attention in post-menopause.
Bone health changes significantly once estrogen drops. Healthy Bones Australia notes that women can lose bone rapidly in the years following menopause, increasing osteoporosis risk over time. The Ministry of Health, New Zealand recommends calcium-rich foods, adequate vitamin D, and weight-bearing exercise as foundations of long-term bone care. Bone density screening or a DEXA scan is worth discussing with your GP if you haven’t already.
Heart health is the other priority. The Australasian Menopause Society identifies cardiovascular disease as the leading cause of death in post-menopausal women, and highlights this as a critical window for prevention. Regular movement, a diet built around whole foods and the Mediterranean diet, maintaining a healthy weight, and monitoring blood pressure and cholesterol all matter more now than they’ve ever done before.
None of these flags are cause for anxiety. They’re simply the areas where early, consistent habits will pay you the biggest long-term dividends.
1. Nutrition that works
Food becomes even more important in post-menopause – not in a restrictive way, by any means, but more of an intentional one.
Fibre is all-important. Most people in Western culture do not get enough, and we need it for gut health and eliminating excess toxins and estrogen. It sounds like a paradox as ovarian estrogen has declined, but xenoestrogens from personal care, cleaning products, food, and the environment need to be excreted rather than recirculated.
Calcium and vitamin D3 are the headline acts for bone health. Good calcium sources include dairy, tofu, almonds, leafy greens, and fortified plant milks. Vitamin D is best assessed with a blood test, since deficiency is common in New Zealand and Australia, particularly during the winter months. In New Zealand, a test will cost around $100 unless you ask your GP to tick the ‘at risk of osteoporosis’ box.
Anti-inflammatory eating patterns support heart health, metabolic balance, and general energy. That means more fatty fish, berries, olive oil, nuts, seeds, and whole grains – less ultra-processed food, excess sugar, and alcohol, all of which can amplify inflammation and disrupt sleep. Or, essentially, the Mediterranean style of eating.

Protein deserves more attention, too, though if you listen to the narrative on social media it will take over your entire life. But muscle mass declines naturally with age, and adequate protein, spread across meals rather than loaded into one, supports muscle maintenance, metabolic health, and satiety. If you’re not active, this is around 1.2g of protein per kg of bodyweight per day, or 1.6kg if you’re more active. Which brings us to:
2. Movement
It’s pretty much common knowledge that physical activity is one of the most effective tools for wellness, and post-menopause is no different. It’s great for bone density, muscle mass, heart health, balance and flexibility, mood, and cognitive function.
But the important thing is to find the right type and duration for you.
Strength training is fantastic. Two to three sessions per week of resistance work – whether that’s weights, resistance bands, Pilates, or bodyweight exercise – supports bone and muscle in ways that cardiovascular exercise alone doesn’t. Walking, swimming, yoga, and cycling all contribute, too. The goal isn’t to be a high-end athlete. It’s about function, longevity, and feeling well in your body for the decades ahead. A big part of it is balance and mobility.
On that note, rebounding is a great choice to add to your repertoire for balance, mobility, weight and – importantly – your lymphatic system. Because the lymphatic system can tighten up at post-menopause.
3. Sleep, stress and mental health
Poor sleep is one of the foundations of how you live in post-menopause. It affects weight, mood, cognition, metabolism, immune function, and how manageable everything else feels. There’s a reason they used sleep deprivation as torture in times of war.
Consistent sleep and wake times, getting out in the morning light without sunglasses, limiting caffeine after midday, reducing screen exposure before bed, and keeping the bedroom cool all support better sleep quality.
Try the rule of 3-2-1: stop eating three hours before bed, quit drinking tea or water (no alcohol or caffeine are no-brainers) two hours prior, and switch off screens one hour before.
Stress management is the other biggie. Chronic stress affects everything, which in turn affects weight, hormonal equilibrium (HPA axis), balance, sleep, and heart health. Whether it’s time outdoors, creative practice, meditation, movement, or simply protecting time with people who restore you, what works is individual. The evidence behind regular mindfulness practice for mood, stress, and even hot flush frequency is reasonably strong and worth knowing about.
Try the 4-7-8 technique: empty your lungs, then slowly breathe in for 4, hold for 7, and exhale for 8. Do this a few times and you will literally feel your body go back into parasympathetic or rest and digest mode (read: relaxed).
4. Supplements: filling the gaps
Wellness and post-menopause health are always about real food first. But post-menopause is a stage where targeted supplemental support can make a difference – particularly where diet alone isn’t meeting shortfalls.
Magnesium is one of the most commonly depleted minerals in midlife women, and it works across sleep quality, muscle function, mood regulation, and bone health. Vitamin D, as noted above, is worth testing and supplementing where levels are low. It’s best paired with vitamin K2. Omega-3 fatty acids support cardiovascular and cognitive health, reduce inflammation, and have evidence around mood – all relevant given the neurological shifts that accompany lower estrogen.
One of your BFF’s forever is part of the Mediterranean diet – extra-virgin olive oil – which has so many benefits for everybody, and especially post-menopausal health.
And we can’t bypass the fact that we created a formula built specifically for post-menopause to fulfill our own needs. Perky Post® combines affron® saffron – which is evidence-backed for improved mood, sleep and emotional wellbeing, with fenugreek, sage, vitamin D3, K2, and resveratrol. It’s designed to support the areas affected by post-menopause: mood, sleep, libido, joint pain, bone health, heart and brain function, and vitality.
And let’s not forget gut health, which we know has a more direct connection to hormonal health than many women realise. The gut microbiome plays a role in how the body processes and recirculates estrogen through a specific group of microbiota known as the estrobolome. So we created Happy Go Tummy®, a synbiotic formula combining award-winning Livaux® gold kiwifruit prebiotic with Lactobacillus rhamnosus to support gut diversity, digestion, mood and immune health.
5. HRT and other medical support
Hormone replacement therapy (now known as menopause hormone therapy, although it’s been slow to catch on) is genuinely helpful for many women – for flushes and sweats, bone protection, and quality of life. It’s not right for everyone, and that decision belongs between a woman and her clinician. What matters is that it’s considered properly rather than dismissed or defaulted to. MenoMe®’s approach is to support women wherever they are – including those on hormone therapy who want to work alongside it with targeted nutrition and lifestyle support.
Vaginal oestrogen and other localised treatments for GSM are also highly effective and underused, which is worth raising with a GP if dryness or discomfort is affecting daily life or intimacy.

6. Sexual health
Vaginal dryness and discomfort during intimacy are common in post-menopause and treatable – yet many women don’t raise it, and many doctors don’t ask. It can be hard to talk about such intimate things, right? Vaginal moisturisers used regularly, water-based lubricants, and localised estrogen treatments are all options worth knowing about. Open communication with your partner helps, too, though it can take practice to have those conversations comfortably, depending on your relationship.
Sexual wellbeing is part of overall wellbeing and post-menopause health. So it deserves the same straightforward attention as bone health or cardiovascular risk.
7. The upside – it’s real
Post-menopause brings freedom from periods, PMS, and pregnancy-related contraception. But the benefits women most consistently report go beyond the practical. Greater confidence. Clearer priorities. Better boundaries. Less tolerance for what doesn’t matter, and more for what does. A sense of having earned something – not just survived the transition, but arrived somewhere with more self-knowledge than before.
Research reflects this. Studies on wellbeing, post-menopauser health and life satisfaction show that many women report improved emotional health in post-menopause compared to the perimenopause years. The hormonal noise dials down. There’s room for something else. Yay!
8. Preventive care – screening that matters
Regular health checks become more important in post-menopause, not less. Bone density or DEXA scans, mammograms, cervical screening, cholesterol, and blood pressure monitoring all help catch changes early when they’re most manageable.
Any post-menopausal bleeding – even minor – should be checked promptly. So should persistent pelvic pain, worsening bladder symptoms, or anything significantly affecting daily life.
FAQs
Do symptoms stop once you reach post-menopause?
Not always. Some improve, while others – including vaginal dryness, sleep disruption, and hot flushes – can continue. The experience varies widely from woman to woman.
Can you still have hot flushes in post-menopause?
Yes. Research shows vasomotor symptoms can persist for several years beyond the final period for many women, though they often become less frequent over time.
NB: For women over 60, hot flushes have been linked with hypertension.
How do you protect bone health after menopause?
Calcium-rich foods, adequate vitamin D3 & K2, weight-bearing and resistance exercise, and bone density or DEXA screening are the key foundations. It’s a good idea to get a complete blood screening panel although be aware that in New Zealand, a vitamin D blood test will set you back approximately $100 unless you ask your GP to tick the box for osteoporosis.
Is HRT suitable for everyone?
No – but that’s not a reason to avoid the conversation. Hormone therapy is effective for many women, but who does well on it depends on individual health history. A GP or menopause specialist can help assess whether it’s an option worth exploring.
The bottom line
Post-menopause is a stage with its own considerations. The women who navigate it best tend to be the ones with good information, targeted support, and a willingness to treat this phase with the same understanding they’d bring to any other significant life transition.
That’s not about overhauling everything at once. It’s about knowing what your body needs, finding what works for you, and building from there. We’re all bioindividuals, so what works for Mary won’t necessarily be great for Jane. Thriving in post-menopause isn’t a lucky outcome. It’s a considered one.
We hope this story helped you! If you have more questions, don’t hesitate to get in touch here.
Just so you know: this article is written by a real person who has studied the physiology of menopause and women’s healthy ageing. While we may use AI as an assistant, the research, insights and heart behind every piece comes from us.

References
- Australasian Menopause Society – menopause.org.au
- Jean Hailes for Women’s Health – jeanhailes.org.au
- Ministry of Health New Zealand – health.govt.nz
- Healthy Bones Australia – healthybones.com.au
- Avis NE et al. Duration of Menopausal Vasomotor Symptoms Over the Menopause Transition. JAMA Internal Medicine.
- Jia Y, Zhou Z, Cao X. Prevalence of poor sleep quality during menopause: a meta-analysis. Sleep and Breathing, 2024.
- Gandhi J et al. Genitourinary syndrome of menopause: an overview of clinical manifestations, pathophysiology, etiologies, evaluation, and management. AJOG.
- The Menopause Society. Genitourinary Syndrome of Menopause.
- Chaikittisilpa et al. Prevalence of female pattern hair loss in postmenopausal wo

 What’s happening in the body?
What’s happening in the body?


